Thousands of patients die each year from the deadly infections lurking in our filthy hospital wards. It’s an epidemic raging out of control, as antibiotics are rendered impotent. “Superbugs” are soaring and they are gathering strength all the time.
Every affluent country in the world where antibiotics are in widespread use is facing the superbug problem, but there is no doubt that it is reaching crisis level in Australia as it already is in Britain and the USA. British hospitals are the most dangerous in Europe for the potentially fatal bug, which prevents wounds from healing. Recent outbreaks in Australian hospitals were out of control necessitating closing wards and operating theatres and cancelling surgery. The main problem was VRE, which is present in many healthy people but can cause serious illness in very sick patients. It can be transmitted on the hands of staff, patients and visitors.
The hospital-acquired infection situation in Australia is no better than England and may even be worse. In 1997 a medical journal reported that patients ‘have more than a 1-in-10 chance of picking up infections in hospital’. A recent report on a related bacterium, MRSA, suggested that some hospitals in Australia lack infection control units (such as isolation units), which are common in the USA. One study on MRSA prevalence in Ireland, and Northern Ireland, found that 700 hospital patients were infected by MRSA during one fortnight in 1999.
A European study suggests that, among European countries, Ireland has one of the poorest records for MRSA infection, with only Italy, Portugal and Greece faring worse. In fact a report of European Anti-Microbial Resistance Surveillance System for 1999 showed prevalence in Ireland which was more than 4 times that of Germany. Proper hand washing, good antibiotic practice, effective ward cleaning and patient isolation are of crucial importance in reducing the spread of MRSA in hospitals. This is of concern for many Irish nurses come to Australia on working holidays and work in our hospitals.
Roll on another 20 years… HAS ANYTHING CHANGED? NO! Superbugs are as deadly as ever.
Off to hospital? To keep an eye on things→ GET A WATCHDOG!
SUPERBUGS HAVE BEEN AIDED BY TWO FACTORS:
- First there is the indiscriminate doling out of antibiotics by doctors over the last 50 years, which has allowed the micro-organisms to develop resistance with deadly efficiency. But even more shockingly…
- …the superbugs have exposed the shameful fact that modern hospitals are simply not clean enough. Instead, they are a breeding ground for infections.
Many wards are filthy and too many medical staff disregard even the most basic rules of hygiene, such as washing their hands between patients. Hospital staff and managers fail to recognize that their disregard for the most basic rules of hygiene is a key factor in allowing this epidemic to take hold.
THE WEAK POINTS:
- Quality of hospital care is a significant problem.
- Infection control surveillance nurses are non-existent.
- Sterilization equipment failures all too common.
- Hospitals disposing of hazardous waste recklessly.
All hospitals must have a mania for cleanliness like Scottish surgeon, Joseph Lister, who virtually “invented” hygiene in the 19th century. Patient safety is and must be paramount.
MAIN CULPRITS
What is C. auris?
Candida auris is a type of fungus or yeast that is a newly emerging health concern. It is multidrug-resistant, meaning it is resistant to many anti fungal drugs that usually treat fungal infections. The fungus first became apparent to researchers in 2009 and has since been causing outbreaks in healthcare settings worldwide.
What is MRSA?
MRSA is a type of germ, which is resistant to a wide range of antibiotics. Like other strains of Staphylococcus, MRSA can live on the skin without causing infection in most people. Hospital patients are especially vulnerable to MRSA and are too weak to fight it off. Staphylococcus aureus can cause actual infection and disease, particularly if there is an opportunity for the bacteria to enter the body, through a cut or an abrasion, for example. But newly emerging strains are causing life-threatening infections in otherwise healthy people. The antibiotic resistance problem arises because bacteria are constantly mutating, creating tiny changes in their genes. In order to stop it spreading you must remember that germs are normally passed by hand. It will normally be spread to patients from someone else in the hospital who has it. Effectively the MRSA bug “hitchhikes” a ride on someone’s hand until it gets to your body. Once it has arrived it prefers to live in wounds. In the pre-antibiotic era, mortality was as high as 90%.
What about MSSA? How serious is it as opposed to MRSA?
MSSA infection, which is also known as Methicillin Sensitive Staphylococcus Aureus, is a disease that we see popping up more and more these days. It’s particularly dangerous and scary for a number of reasons. The first reason is because it is most commonly contracted while at hospitals, when a person is often in a weakened condition. The second reason it’s scary is because it’s resistant and sensitive to powerful antibiotics, making it especially tricky and difficult to eradicate. MSSA and MRSA infection are virtually the same extremely dangerous disease, with minor differences, because they both are antibiotic resistant and generally are contracted hiding out at hospitals. The most famous case of a patient contracting one of these diseases in hospital is British actress Leslie Ash, who found herself paralyzed once an MSSA infection attacked her spinal tissue, which was introduced through an epidural injection.
Staph infection can invade the body through a number of channels. Most commonly, it inhabits the soft tissues of the nasal cavity, the respiratory tract, as well as open wounds. Depending on the area infected, staph will often manifest itself as red bumps, which ultimately grow into painful boils. Fever and rashes often accompany the boils. When MSSA is introduced into either a wound, or else into healthy tissue somewhere inside the body from either shots or surgery, the symptoms and effects of the disease may be enhanced. Paralysis of the lower half of the body is very common, along with lasting pain in the area where the infection occurs. After MSSA infects the body in a specific region of tissue, it begins to grow and becomes very difficult to eradicate. Often large portions of tissue must be cut away and heavy doses of antibiotics.
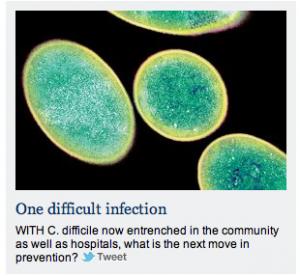
What is C. difficile?
Clostridium difficile is a spore-forming bacterium, which is present as one of the “normal” bacteria in the gut of up to 3% of healthy adults. C.difficile is much more common in babies – up to two thirds of infants may have it in the gut, where it rarely causes problems. People over 65 are more susceptible to infection. It can cause illness when certain antibiotics disturb the balance of normal bacteria. Its effects can range from nothing in some cases to diarrhoea or severe, life-threatening, inflammation of the bowel.
What is GRE?
Glycopeptide-resistant Enterococci, are commonly found in the bowels of most people. There are many different species, but only a few can cause infections in humans – 95% of infections are caused by Enterococcus faecium and Enterococcus faecalis. These species are the two most common strains of GRE, which are resistant to glycopeptide antibiotics (vancomycin and teicoplanin). GRE commonly cause wound infections, blood poisoning and infections of the abdomen and pelvis.
Already had staph?
If you know that you have had Staphylococcus then you should tell your doctor and also inform the hospital if you are re-admitted. Hospitals may very well discriminate against you by refusing to admit you but you have a duty to your fellow patients to disclose it. You also have the right to demand of a hospital to be isolated away from the main ward area and if the hospital will not accommodate you indicates they have no infection-control protocols in place.
SOME OF THE SUPERBUGS
- C. AURIS: Candida auris is a fungal disease – can spread in hospitals and cause invasive infections.
- MRSA: Methicillin-resistant Staphylococcus aureus – once curable by penicillin.
- MSSA: Methicillin-sensitive Staphylococcus aureus – is susceptible to methicillin, i.e. not resistant.
- C. DIFFICILE: Clostridium difficile – worst episode caused the deaths of 65 patients at one hospital – no patient was isolated – reckless and criminal disregard for basic hygiene.
- GRE: Glycopeptide-resistant Enterococci.
- VRE: Vancomycin-resistant Enterococcus. First case in Australia reported in 1994.
- MDR-AB: Multi drug-resistant Acinetobacter baumannii.
- MDR-TB: Multi drug-resistant tuberculosis – most of TB germs are MDR.
- TB: Tuberculosis commonly affects the lungs. More than 1,100 new cases diagnosed in Australia in 2010. Countries such as India, where the disease is prevalent, had 1.23 million cases in 2010, 2,967 of those MDR cases.
- XDR-TB: Extremely drug-resistant tuberculosis – lethal new form of TB and virtually impossible to cure which has exploded in Africa, Asia and Russia.
- KPC: Klebsiella pneumoniae carbapenemase – resistant to most of the common antibiotics in Brazil.
THE LATEST SUPERBUG TO JOIN THE “SUPERBUG CLUB”?
- HO41: Gonorrhea is the second most common sexually transmitted infection in North America. It has the potential to be as deadly as the AIDS virus. This particular strain of gonorrhea was discovered in Japan two years ago. HO41 has so far proved resistant to current antibiotic treatment, so it has been placed in the superbug category (2 May 2013).
ANTIBIOTIC RESISTANT DISEASES AROUND THE WORLD
MRSA
- The first reported case of MRSA in Australia was in 1968.
- It now accounts for 15-20% of all staphylococcus aureus infections in Australia, with a median 35% mortality rate.
- About 6,900 episodes of staphylococcus aureus bacteraemia occur in Australia annually.
- In pre-antibiotic era, mortality was a high as 90%.
- MRSA is used to describe a number of strains of the bacteria staphylococcus aureus, which are resistant to a number of antibiotics, including methicillin.
- Staphylococcus aureus is a group of bacteria that live on the surface of people’s skin and inside the nose and can be spread through contact.
- Problems occur if bacteria enter the body through cut of wound.
- People with weakened immune systems or who have undergone surgery can develop more serious problems.
VRE BACTERIA
- Since 1988, resistance to vancomycin has emerged and increased worldwide.
- The first case was reported in Australia in 1994. A 1998 report on the emergence of VRE here documented 69 cases.
- The simple enterococci germ is generally harmless, living in the intestines of most people.
- Vancomycin is an antibiotic used to treat serious infections, and VRE bacteria has become resistant to the antibiotic,
- Patients at risk of developing VRE infections have typically suffered from a long-term illness, undertaken different courses of antibiotics, had major surgery, treated for serious conditions such as cancer, had organ transplant, been in intensive care, or treated with a course of vancomycin in the past.
- VRE is spread by touch and can be prevented with regular and thorough hand washing, particularly after going to the lavatory.
TUBERCULOSIS
- Commonly known as TB, tuberculosis is an infectious bacterial disease, most commonly affecting the lungs. It is transmitted through phlegm of people infected with the disease.
- More than 1,100 new cases of TB were diagnosed in Australia in 2010 – 33 of them with the multi-drug resistant strain.
- Countries such as India, where the disease is prevalent, had 1.23 million in 2010 – 2,967 of those MDR cases.
- Anti-tuberculosis drug resistance is a major public health problem threatening progress made in TB care and control worldwide.
- Drug resistance arises due to improper use of antibiotics in chemotherapy of drug-susceptible TB patients.
- Essentially, drug resistance arises in areas with weak TB control programs.
ONE EXAMPLE OF INFECTION CONTROL FAILURE AT ROYAL PERTH HOSPITAL, WESTERN AUSTRALIA
- Man admitted to hospital for total knee replacement
- Acquires post-operative staph infection
- Has more surgery to wash out knee infection
- Then more surgery to re-do knee replacement
- Acquires another post-operative infection
- More surgery to wash out knee infection
- Drugs Chart disappears from patient’s medical record
- Knee replacement removed altogether and knee fused straight
- 10 day hospital stay became 16 weeks
- Man left a cripple with knee stiff like concrete
- RPH denies negligence, of course.
CLEAN UP YOUR ACT is the main advice we give hospitals!
THE GOOD SIDE OF BACTERIA
A recent feature in “Scientific American” magazine reported on the latest findings on microbiomes. This is the name given to the trillions of bacterial cells that inhabit our mouths, intestines, genitals and skin.
The number of bacteria we host outnumbers human cells by a factor of 10-to-1. They vary from being pathogenic (disease causing) or benign to actively benevolent for our bodies.
There are some particularly helpful bugs. Bacteriodes thetalotaomicron creates over 260 enzymes that digest plant material, allowing us to extract nutrients from potatoes and other vegetables. Other bacteria assist our immune system, reducing the risk of disease.